Eczema | Symptoms | Causes | Prevention | Treatment |
Eczema is a term for a group of conditions that cause the skin to become inflamed and itchy. Some types of eczema can cause blisters and the skin may crack and bleed.
The word “eczema” comes from the Greek word “ezkein” which means “break out”. Often it is used to refer to atopic dermatitis, which is the most common type of eczema. It is also sometimes used to refer to contact dermatitis.
Eczema is not contagious. It is caused by a combination of genetics, environmental triggers, and immune system activation.
In many cases, eczema can flare periodically and then clear up, often for long periods of time. People with the condition can spend up to three hours per day treating the symptoms, and it can interfere with their daily lives.
There are several types of eczema. These include allergic, irritant, contact, and nummular eczema.
The first signs of eczema are itchiness and redness. The itchiness comes before the rash, leading to eczema sometimes being called an “itch that rashes”. During the night, the itchiness is often at its most severe.
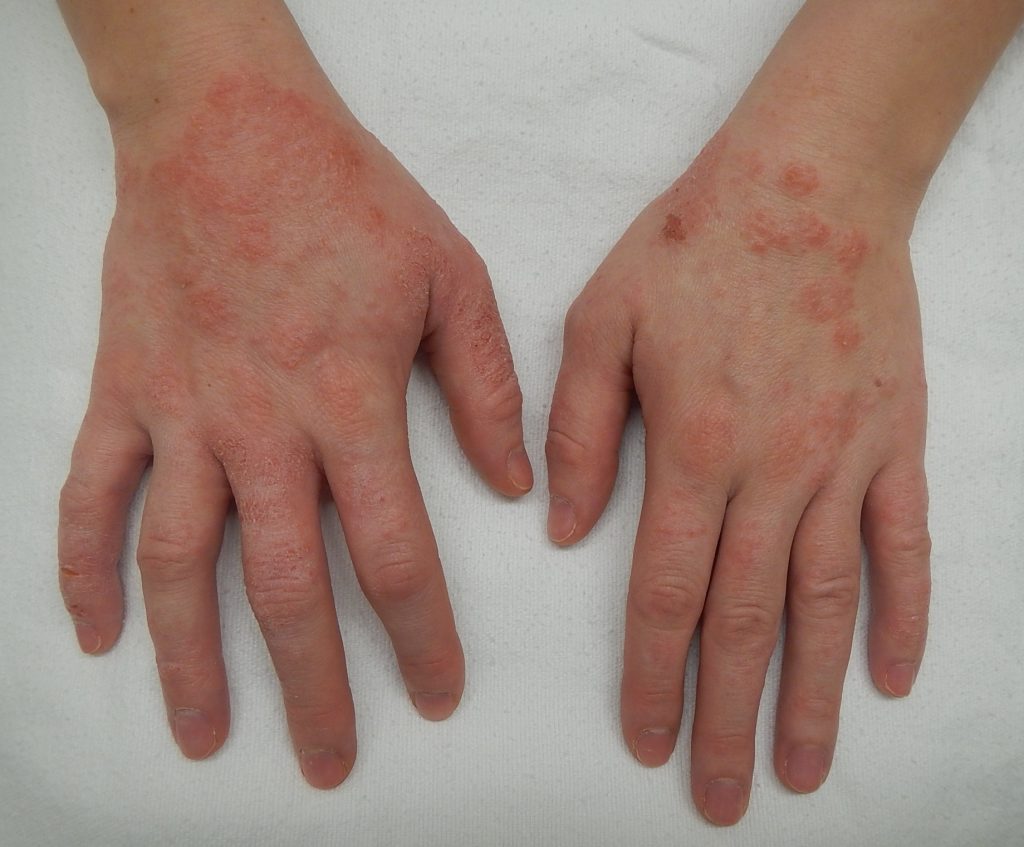
The skin can become inflamed and irritated. These red patches can appear on the hands, feet, neck, and eyelids.
Eczema can also cause bumps on the skin. The bumps can leak when scratched and repeated scratching can in turn cause the skin to crack.
While it can occur at any age, eczema is common in children. In babies and infants, it tends to appear on the scalp and face. In infants, the rash can ooze and crust over. As toddlers become mobile, the symptoms becomes more localised.
Along with the hands, the rash can be seen on the inner elbows, the back of the knees, and the back of the necks. In adults, eczema can present as scaly, dry patches. The skin may also become discolored or thickened.
Eczema can affect the skin pigments in darker-skinned people. This can result in the affected areas turning darker or even lighter.
Eczema may cause permanent discoloration and thickening of the skin even after a flare up subsides. Many people suffering from this condition feel self-conscious about their skin. This chronic skin condition can flare up, followed by a period of calm skin, and then flare up again.
The specific cause of eczema is unknown.
Eczema is more common in children who have a family history of allergies, asthma, or hay fever (allergenic rhinitis). It is also more common in adults who develop these conditions before they are 30 years old. Both males and females are equally affected by this chronic skin condition.
Healthy skin helps to retain moisture and provides protection from irritants and allergens.
Eczema is related to a gene variation that reduces the skin’s ability to provide protection. Research shows that this variation occurs in the gene that creates the protein filaggrin. Filaggrin helps our body maintain a protective layer on top of the skin. A reduction in filaggrin leads to moisture loss and allows the entry of bacteria and viruses.
This variation in the filaggrin gene leads to eczema in up to a third of people who have North European and Eastern Asian ethnicity. Along with genetic factors, the skin’s ability to provide protection can also be caused by environmental factors.
Eczema is thought to be triggered by an overactive immune system that responds aggressively to irritants.
In people with eczema, the immune system cannot tell the difference between the body’s proteins and the proteins of bacteria or viruses. This leads to inflammation which causes the red, itchy patches typical of the condition.
Also, some bacteria contain proteins called proteases and can trigger eczema. This type of protein harms the skin barrier by breaking the connection between skin cells. This in turn causes dry skin that can set off a flare up.
Our bodies contain colonies of harmless bacteria called microbiota. These bacteria contribute to the body’s natural processes. They also have a positive effect on our health. Probiotics can help keep microbiota in balance.
However, an imbalance in any of these bacterial colonies, usually in the gastrointestinal tract, can cause dysbiosis. Dysbiosis can also occur on the skin. It may also play a role in the development of atopic dermatitis and eczema in early life.
Dysbiosis of the gut microbiome and immune system imbalances persist into adult life and contribute to both conditions.
Some women may develop eczema or experience increased symptoms during pregnancy. This occurs due to changing hormone levels.
Allergens cause an allergic reaction and can irritate the skin leading to inflammation. Some types of fabrics, skin products, and soaps can trigger eczema. Other examples of allergens include dust mites, air pollutants, pollen, and mold. People with this skin condition can experience flares from mild irritants as well.
Irritants that can trigger a flare up include personal and every day products such as hand soap, shampoo, and disinfectants. Even natural products like fruit and vegetable juices can cause irritation.
Certain foods such as eggs, dairy items, nuts and seeds can cause a flare up of eczema. Ingredients like soy and wheat can also be a trigger.
While emotional problems do not cause eczema, stress and anxiety can worsen the symptoms. Hot and cold temperature extremes can lead to flare ups too. Heat can cause sweating which can make itchiness worse. Dry air during the winter make the skin dry.
Repeated handwashing and drying can also trigger the symptoms of this condition. Eczema flare ups can occur sometime after exposure to a trigger. This lag time can make it difficult to identify specific triggers.
Moisturizers help improve the skin barrier. Use moisturizers throughout the day or at least twice daily. Choose products without fragrances to minimize reactions.
Apply medicated lotions, ointments or creams to seal in moisture. Some research indicates that creams with vitamin B12, coconut oil, and sunflower oil may help keep the skin moisturized.
Follow a regular bathing and moisturizing schedule. Limit showers and baths to 10 to 15 minutes. Use warm instead of hot water. Wash with gentle soaps to avoid triggering a flare up.
Pat your skin dry gently after bathing. Use a soft towel to reduce rubbing of the skin. Apply moisturizer while your skin is still a bit damp to lock in moisture.
Scratching and rubbing itchy patches can cause skin infections. Wear soft, breathable fabrics to reduce itchiness. Maintain short and smooth nails to reduce skin damage during scratching.
Avoid known triggers and identify potential ones to reduce flare ups.
Foods such as eggs, milk, wheat and soy can cause eczema flares in infants and children. While common allergic foods may cause the condition in children, this is not the case for adults.
For adults with eczema, avoid exposure to chemicals in household and personal products. Certain fabrics and detergents can also cause the condition to worsen. Wash any new clothes before you wear them.
Keep your home free from house dust mites. These microscopic organisms have been associated with eczema. Avoid intense physical activities during a flare up. Sweat can increase itchiness and scratching. Take a shower immediately after swimming outdoors or in pools to remove chemicals from your skin.
Stress reduction and a sleep routine can reduce the chances of flare-ups. Learning to recognize and cope with stressful situations can also help. Eczema can cause anxiety and self-consciousness. Stress reduction techniques can relieve anxiety and stop this skin condition from worsening.
There is no cure for eczema. With the right treatment plan, its symptoms can be managed effectively.
A treatment plan for this condition takes into account the patient’s age and symptoms. The aim of a treatment plan is to heal the skin and minimize flare ups. It may focus on moisturizers, medications, and trigger elimination.
There are many treatment options and new ones are being developed. Since responses to each treatment may be different, it is best to discuss options with your healthcare practitioner.
Eczema treatment requires consistent use of over the counter and prescription medications. Monitor your skin for changes, infections, and improvements.
“Atopic dermatitis (eczema)”
“Eczema: Symptoms, Causes, and Treatment”
“Eczema”
“What to know about eczema”
“What Causes Dysbiosis and How Is It Treated?”
“Microbiome in the Gut-Skin Axis in Atopic Dermatitis”